Brucellosis*
Bacteria
Bacteria
| Genus Species | Brucella (B. melitensis, B. abortus, B. suis, B. canis ) |
| Host Range | Infected animals (swine, cattle, goats, sheep, dogs) |
| Transmission | Skin or mucous membrane contact with infected animals, their blood, tissue, and other body fluids |
| Symptoms | High and protracted (extended) fever. Infection affects bone, heart, gallbladder, kidney, spleen, and causes highly disseminated lesions and abscess |
| Incubation | 1-15 weeks |
| Fact | Most commonly reported U.S. laboratory-associated bacterial infection in man |
| Treatment | Antibiotic combination: streptomycina, tetracycline, and sulfonamides |

Salmonellosis
Bacteria
Bacteria
| Genus Species | Salmonella (S. cholera-suis, S. enteriditis, S. typhymurium, S. typhi) |
| Host Range | Domestic (dogs, cats, monkeys, rodents, laboratory rodents, rep-tiles [especially “turtles], chickens and fish) and herd animals” (cattle, chickens, pigs) |
| Transmission | Direct contact as well as indirect consumption (eggs, food vehicles using eggs, etc.). Human to “human transmission also possible” |
| Symptoms | Mild gastroenteritiis (diarrhea) to high fever, severe headache, and spleen enlargement. May lead to focal infection in any organ or tissue of the body) |
| Incubation | 6 hours to 3 days |
| Fact | Fatality rate of 5-10% |
| Treatment | Antibiotic combination: chloramphenicol, neomycin, ampicillin |
Shigellosis*
Bacteria
Bacteria
| Genus Species | All Shigella species |
| Host Range | Captive non-human primates |
| Transmission | Oral-fecal route |
| Symptoms | Ranges from asymptomatic carrier to severe bacillary dysentery with high fevers, weakness, severe abdominal cramps, prostration, edema of the “face and neck, and diarrhea with blood, mucous and inflammatory” cells |
| Incubation | Varies by species. 16 hours to 7 days. |
| Fact | Highly infective. Low number of organisms capable of causing infection. Rate of “infection in imported monkeys can be high” |
| Treatment | Intravenous fluids and electrolytes, Antibiotics: amoxicillin, “trimethoprin- sulfamethoxazole” |

Leptospirosis
Bacteria
Bacteria
| Genus Species | Leptospira interrogans |
| Host Range | Animal, human urine |
| Transmission | Direct contact with urine of infected dogs, mice or rats. Indirect contact with urine “contaminated materials. Droplet transmission via” aerosols of urine |
| Symptoms | Phase 1: headache, muscle ache, eye pain with bright lights, chills and fever. Phase 2: fever with stiffness of the neck and inflammation of the nerves to the eyes, brain, spinal column |
| Incubation | 7-12 Days |
| Fact | Leptospirosis associated with liver and kidney disease is “called Weil’s syndrome,” characterized by jaundice |
| Treatment | Doxycycline and penicillin. Severely ill patients may need IV “fluids, antibiotics and dialysis” |

Relapsing fever
Bacteria
Bacteria
| Genus Species | Borreliae spp. [B. recurrentis (louse- borne), B. hemsii (tick-borne)] |
| Host Range | Animals |
| Transmission | Tick-borne, blood transfusions |
| Symptoms | Fever, headache and muscle pain that lasts 4-10 days and subsides. Afebrile period lasting 5-6 days followed by a recurrence of acute symptoms |
| Incubation | 5-15 days |
| Fact | Epidemic relapsing fever (transmitted by lice) is more severe than endemic relapsing fever (transmitted by ticks) |
| Treatment | Tetracyclines, chloramphenicol |
Tuberculosis
Bacteria
Bacteria
| Genus Species | Mycobacterium tuberculosis |
| Host Range | Primarily humans, cattle, non-human primates, other animals (rodents) |
| Transmission | Inhalation of aerosol droplets, contaminated equipment, bites |
| Symptoms | Ranges from fever and fatigue to chronic pulmonary disease (fatal). Lungs, kidney, vasculature (affects all parts of body) |
| Incubation | 2-5 weeks |
| Fact | Multidrug-resistant TB (MDR TB) is an infection resistant to at least two first-line anti- TB drugs, isoniazid and rifampicin |
| Treatment | Isoniazid, rifampin, streptomycin, and ethambutol |
Melioidosis*
Bacteria
Bacteria
| Genus Species | Burkholderia pseudomallei ( formerly Pseudomonas pseudomallei ) |
| Host Range | Equines, especially horses and mules; humans are accidental hosts |
| Transmission | Transmitted by inhaling dust contaminated by the bacteria and when contaminated soil comes in contact with abraded skin |
| Symptoms | Cholera-like symptoms (fever, chills, prostration). Skin lesions, swollen lymph glands, abscesses septicemia or pneumonia |
| Incubation | 2-4 days |
| Fact | Relatively uncommon disease for humans, but when left untreated, has 95% fatality rate |
| Treatment | Chloramphenicol, doxycycline, sulfisoxazole, or cotrimoxazole. IV chloramphenicol for bacteremia |
Tularemia*
Bacteria
Bacteria
| Genus Species | Francisella tularensis |
| Host Range | Isolated from 100 species of wild animals (e.g., rabbits, skunk), 9 domestic mammals, 25 species of birds, frogs, and reptiles |
| Transmission | Arthropods, direct or indirect contact, ingestion of contaminated meats, inhalation of dust, materials contaminated with urine, feces or tissues, bites and scratches |
| Symptoms | High fever, chills, headache, focal ulcers, swollen lymph nodes |
| Incubation | 1-10 days |
| Fact | Bacterium formerly known as Pasteurella tularensis |
| Treatment | Streptomycin, tetracycline |
Herpesvirus
Virus
Virus
| Genus Species | Herpesvirus Type 1 (fever blister, cold sore) and Type 2 (genital herpes), Herpesvirus hominis, Herpes simiae (Herpes B) |
| Host Range | Human, non-human primates |
| Transmission | Produce latent infections in host and frequently shed without overt lesions |
| Symptoms | Frequently asymptomatic. May have vesicular lesions, neurological or flu- like symptoms |
| Incubation | 5 days to 1 month |
| Fact | Herpes simiae is 100% fatal if untreated; Herpes Types 1 and 2 are not fatal but cause chronic infection from recurrences |
| Treatment | Acyclovir or valcyclovir will arrest the virus but will not eliminate virus from the host |
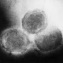
Poxvirus*
Virus
Virus
| Genus Species | Monkeypox, vaccinia, cowpox, buffalopox, cantagalo, and aracatuba viruses |
| Host Range | Non-human primates, swine, cattle, horses, birds |
| Transmission | Direct skin contact with lesions on infected animals |
| Symptoms | Localized lesions, rash, fever, sore throat, malaise, encephalitis |
| Incubation | Generally: 5-10 days after infection |
| Fact | Poxviruses are the largest and most complex viruses |
| Treatment | smallpox vaccine, cidofovir, and vaccinia immune globulin (VIG) |

Rabies Virus
Virus
Virus
| Genus Species | Rhabdoviridae, genus Lyssavirus |
| Host Range | Natural reservoir: bats. All mammals: wild animals (raccoons, rodents, foxes, etc.) “domestic animals (dogs, cats) and” humans |
| Transmission | Animal bite, contact with infected saliva or tissue |
| Symptoms | Headache, fever, malaise, nervousness, dilation of pupils, salivation, excessive perspiration, insomnia, paralysis of throat “muscles, inability to swallow, convulsions, seizures, generalized” paralysis and death |
| Incubation | 3-8 weeks |
| Fact | Untreated, the fatality rate is 100%; Post- exposure treatment is effective until day 6 post- infection |
| Treatment | Antirabies vaccine before clinical onset of symptoms; post-exposure treatment “with rabies immune globulin & vaccine” |
Viral Hemorrhagic Fever*
Virus
Virus
| Genus Species | Multiple species: Filoviridae ; Ebola virus, Lassa virus, Marburg virus |
| Host Range | Humans, non-human primates (Cynomolgous monkeys) |
| Transmission | Contact with blood and body fluids of infected animals |
| Symptoms | Severe fever, sore throat, cough, diarrhea, vomiting, hemorrhage and death |
| Incubation | 2-21 days (5-12 days in most cases) |
| Fact | 50-90% fatality rate for Ebola virus; 25% mortality rate for Marburg virus; 15-20% mortality for Lassa fever virus |
| Treatment | No vaccines; Treatment directed at maintaining renal function, electrolyte “balance and combating hemorrhage and” shock |

Arboviral infections*
Virus
Virus
| Genus Species | Multiple species: Togaviridae, Flaviviridae, Bunyaviridae, Arenaviridae |
| Host Range | Ticks, insects, infected animals (deer, birds, rodents, etc.) |
| Transmission | Ticks, insects, blood transfusion |
| Symptoms | Various: viremia, lymphadenapothy leading to systemic infection. Can involve CNS (encephalitis), skin/bone marrow/blood vessels (hemorrhagic fevers) |
| Incubation | Multiple Ranges; 14-25 days (Avg. 18 days) post infection |
| Fact | Causes: Rift Valley fever, Denque fever, Yellow fever; Sandfly (Hantavirus) fever; Omsk hemorrhagic fever, and West Nile virus infections |
| Treatment | No vaccines for most (except yellow fever virus), no known antivirals; supportive treatment only |
Viral Hepatitis
Virus
Virus
| Genus Species | Hepatitis A, B, C, D (delta), E, F, G |
| Host Range | Humans, non-human primates (chimpanzee, wooly monkey, gorilla, “Celebes ape, some marmosets” |
| Transmission | Close contact with infected animals or materials |
| Symptoms | Fever, anorexia, vague abdominal discomfort, nausea and vomiting, sometimes arthralgias and rash, “often progressing to jaundice; fever may be absent or mild” |
| Incubation | 3-6 weeks |
| Fact | Hepatitis A has no carrier state; Hepatitis B 20% chronic; “Hepatitis C 85% chronic” |
| Treatment | Vaccines for Hepatitis A and B only. Treatment with alpha “inter-feron and intra-venous immuno-” globulins (HBIG) |
Lymphocytic Choriomeningitis (LCM)
Virus
Virus
| Genus Species | Multiple arenaviruses |
| Host Range | Rodents (hamsters, mice, guinea pigs), monkeys and humans |
| Transmission | Infected mice excrete virus in saliva, urine and feces; man infected through inhalation of aerosolized particles of (urine, feces or saliva) contaminated with virus |
| Symptoms | Biphasic febrile illness, mild influenza like illness or occasionally meningeal or meningoencephalomyelitic symptoms, transverse myelitis |
| Incubation | 15-21 days |
| Fact | 46 documented laboratory-acquired cases with 5 deaths; cases also reported arising from contaminated cell lines |
| Treatment | No specific treatment; anti-inflammatory drugs may be useful; No known vaccines |

Vesicular Stomatitis*
Virus
Virus
| Genus Species | Multiple strains of Vesicular Stomatitis Virus (VSV) Rhabdoviridiae |
| Host Range | Bovine, equine, porcine animals. |
| Transmission | Probably arthropod-borne via the bite of an infected sandfly, mosquito or blackfly; by direct contact with infected animals (vesicular fluid, saliva) |
| Symptoms | Infuenza-like illness, malaise, fever, headache, nausea and vomiting |
| Incubation | 24-48 hours |
| Fact | Documented hazard to personnel (45 laboratory-acquired infections before 1980) handling infected livestock, tissues and virulent isolates |
| Treatment | Virus is self-limiting and illness is short in duration. (3-6 days) |

Sub-viral Agents and Related Diseases (i.e., Scrapie)*
non-RNA/DNA Infectious Protein Virus- like particle
non-RNA/DNA Infectious Protein Virus- like particle
| Genus Species | Transmissable Spongiform Encephalopathies (TSE): BSE and vCJD (vCreutzfeld- Jacob Disease) |
| Host Range | Adult sheep goats, and cows can infect humans |
| Transmission | Ingestion or handling of brain tissue or unfixed brain cells from infected animals |
| Symptoms | Degeneration of the nervous system, severe variable alteration of the grey matter of the brain |
| Incubation | 2-5 years |
| Fact | The agent responsible for TSE’s is smaller than the smallest known virus and has not been completely characterized |
| Treatment | There are no known treatments or vaccines for these TSE’s |

Amoebic Dysentery
Parasite (protozoa)
Parasite (protozoa)
| Genus Species | Entamoeba histolytica |
| Host Range | Monkeys can readily transmit the agent to humans |
| Transmission | Food, water, fomites, insects. Fecal-oral route. Cyst is resistant to drying |
| Symptoms |
Frequent passage of feces/stool, loose stools and vomiting. Variations depending on parasites. Can be frequent urge with high or low volume of stool, with or without some associated mucus and even blood |
| Incubation | 2 days to several months to even years |
| Fact | Harmless amoebas can live in the intestines for years without causing symptoms. Attacks can last from a few days to weeks |
| Treatment | Antiamebic drugs (Iodoquinol, metronidazole) and antibiotics to treat associated bacterial infections |
Giardiasis
Giardiasis
Giardiasis
| Genus Species | Giardia lamblia |
| Host Range | Dogs, monkeys |
| Transmission | Drinking contaminated water, person-to-person “contact, eating contaminated food, and” direct contact with infected animals |
| Symptoms | Ranges from asymptomatic to nausea, fatigue, anorexia, severe diarrhea and high fever |
| Incubation | 3-25 days |
| Fact | Most common waterborne diarrheal disease in humans |
| Treatment | Quinacrine hydrochloride, “metronidazole, tinidazole,” albendazole and furazolidone |

Balantadidiasis
Parasite (protozoa)
Parasite (protozoa)
| Genus Species | Balantidium coli |
| Host Range | Monkeys, pigs, and other nonhuman primates readily transmitted to humans |
| Transmission | Direct contact with feces, person-to-person transmission |
| Symptoms | Ranges from asymptomatic to severe diarrhea |
| Incubation | 4-5 days |
| Fact | Cysts survive for long periods in the environment |
| Treatment | Tetracycline, Iodoquinol, metronidazole |
Malaria
Parasite (protozoa)
Parasite (protozoa)
| Genus Species | Plasmodium species: P. falciparum “P. vivax P. ovale P. malariae” |
| Host Range | Anopheles mosquito |
| Transmission | Mosquito bite |
| Symptoms | Fever, chills sweating, headache, nausea, vomiting, muscle pain, anemia, bloody stools, jaundice, convulsion, coma |
| Incubation | 10 days to 4 weeks after infection; symptoms then cycle every 48 days |
| Fact | A malaria vaccine has been developed and is being tested in Africa. Results are promising |
| Treatment | Chloroquine, primaquine phosphate, Malorone |

Toxoplasmosis
Parasite (protozoa)
Parasite (protozoa)
| Genus Species | Toxoplasma gondii |
| Host Range | Amazing lack of host specificity. Primates, “carnivores (felines), rodents, birds, undulates” |
| Transmission | Consuming under-cooked infected meats; ingestion “of oocysts in milk, food or water; inhalation of oocysts;-contact with soil” containing contaminated cat feces; |
| Symptoms | Localized lymphadenopathy accompanied with fever, sore throat, rash, pneumonitis, myocarditis, and encephalitis |
| Incubation | 10-23 days following “ingestion of contaminated meats, or” inhalation of aerosols |
| Fact | Affects one third of the human race. “Especially infective to immunosupressed individuals” |
| Treatment | Sulfonomides (sulfadiazene, “sulfamerazine, sulfamethazine), pyrimethamine” |
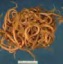
Ascariasis (Roundworm)
Nematode
Nematode
| Genus Species | Multiple Ascaris species (A. lumbricoides, A. suum ) |
| Host Range | Pigs; Humans are the definitive host |
| Transmission | Ingestion of contaminated food or water |
| Symptoms | Lung damage, intestinal symptoms |
| Incubation | 4 to 8 weeks |
| Fact | Ascaris lumbricoidesis the “largest and, globally, the most widespread of all human intestinal” roundworms |
| Treatment | Pyrantel pamoate, mebendazole, surgery for removal in lung tissue |
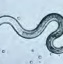
Visceral Larval Migrans (VLM)
Nematode
Nematode
| Genus Species | Nematodes of the Toxocara genus (T. canis, T. felis ) |
| Host Range | Dogs, cats |
| Transmission | Ingestion of eggs through direct contact with feces or contaminated materials |
| Symptoms | Fever, cough, wheezing, itching/irritation associated with migration of nematodes into tissues. Ocular migration may cause blindness |
| Incubation | 4 to 7 weeks |
| Fact | More than 80% of all puppies in the U.S. are infected with this nematode |
| Treatment | Usually a self-limiting disease–treatment only given in severe cases (glucocorticoids and bronchodilators for pulmonary disease) |

Strongyloidiasis
Nematode
Nematode
| Genus Species | Strongyloides stercoralis |
| Host Range | Dogs, cats, monkeys |
| Transmission | Careless handling of contaminated fecal materials |
| Symptoms | Abdominal pain, diarrhea, and rash. Less commonly, nausea, vomiting, weight loss and cough. Severe infection can cause severe tissue damage, systemic damage of various tissues in the body and potential death |
| Incubation | skin 7 hours; lung 1 week; intestines 2 wks; average 4-21 days |
| Fact | The parasite penetrates the skin and migrates to the lungs. Then it travels up to the mouth and is swallowed into the intestinal tract |
| Treatment | Ivermectin with Albendazole as the alternative |
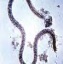
Trichinosis
Nematode
Nematode
| Genus Species | Trichinella spiralis |
| Host Range | Generally pigs or cattle |
| Transmission | Eating undercooked flesh of animals infected with the larvae |
| Symptoms | Nausea, vomiting, diarrhea, fever, neurological disorders, possible cardiac involvement |
| Incubation | Abdominal symptoms: 1- 2 days. “Further symptoms 2-8” weeks after infection |
| Fact | Over 100 species of animals may be a host of this parasite |
| Treatment | Thiabendazole (Mintezol), Albendazole “(Albenza), Mebendazole” (Vermox), Prednisone |
*Images were obtained from the U.S. Centers for Disease Control & Prevention Public Health Image Library (PHIL). 08/2008
